Identification and treatment of dyslipidemia is necessary to reduce the rate of atherosclerosis and the subsequent cardiovascular events, including coronary artery disease (CAD), which may be pharmacologic or non pharmacologic. Patients with abnormal lipid profiles (dyslipidemia) shall be identified and treated on the basis of patients’ risk profiles.
Important points regarding the diagnosis of dyslipidemia:
- From the age of 20 everyone shall be screened for dyslipidemia every 5 years including those who have a normal lipid profile.
- But those who are obese and having other risk factors including positive family history for dyslipidemia and those with CAD, should perform annual screening.
- Fasting serum lipid profile is normally preferred.
- Subject shall be screened for the metabolic causes of dyslipidemia, including diabetes mellitus (DM), liver diseases, hypothyroidism, and nephrotic syndrome.
- Patient medication history shall also be assessed, because medications containing progestins, corticosteroids, or anabolic steroids can lead to dyslipidemia.
Risk Assessment?
Patients with established coronary heart disease (CHD) and those with a risk of developing CHD must be considered for lipid-lowering therapy
- CHD or equivalent
patients (>20%) with a 10 – year risk of CHD, having DM or Peripheral Vascular Disease or abdominal aortic aneurysm, or CAD.
- CHD risk factors
Family history of developing CAD (age <55 for men, <65 for women), or low serum high density lipoprotein HDL (age <45 for men, <55 for women), or hypertension, or smoking, or age( >45 for men, <55 for women).
Initiation of therapy and the ideal goal for LDL and non-HDL levels:
- The ideal LDL goal for CAD or equivalent patients, shall be <100 (or <70) and the non-HDL goal shall be <130 while initiation of the therapy shall be regardless of LDL level in the body.
- Patients having 0-1 risk factors for developing CHD will have an ideal goal for LDL as ( <160), and non-HDL as (<190) while for initiation of the therapy the LDL level must be >190.
- Patients having 2+ risk factors for developing CHD will have an ideal goal for LDL as ( <130), and non-HDL as (<160) while for initiation of the therapy the patient must have a 10-year risk and 10-20% LDL as >130 or a 10year risk and <10%LDL as >160
Life style changes required for therapy:
- life style modifications, as described below, are advised to be followed, for at least 6 weeks, before initiating pharmacotheraphy.
- <7% of Calories shall be obtained from saturated fat on a daily maintenance basis
- Out of the total calories not more than 25-35% must be obtained from total fat
- Intake of monounsaturated fats and polyunsaturated fats must be increased.
- monounsaturated fats up to 10 % of the total caloric intake
- polyunsaturated fats up to 20 % of the total caloric intake
- total daily cholesterol shall not be consumed more than 200mg
- exercise and weight loss may be beneficial up to some extent
- health diet containing plant sterols, Omega-3 fatty acids, and a viscous fiber shall be consumed
Pharmacotherapy:
HMG-CoA reductase inhibitors (statins):
- can lower LDL by 18-55% and Triglycerides by 7-30%
- can increase HDL by 15%
- check baseline LFTs three months after initiating therapy , discontinue therapy if LFTs>3 times the upper limit of normal
- keep in view the ADRs and efficacy of every agent
BileAcid Sequestrants:
- decrease LDL by 15-30%
- increase HDL by 3-5%
- lower or no effect on TGs
- GI upset and decrease absorption of other medications are ADRs
Nicotinic Acid:
- decrease LDL by 5-25%
- increase HDL by 15-35%
- decrease TGs by 20-50%
- contraindicated in gout, CLD, or diabetes relatively
Fibrates:
- decrease LDL by 5-20%
- increase HDL by 10-35%
- decrease TGs by 20-50%
- dyspepsia, myopathy etc are the ADRs
Ezatimibe:
- decrease LDL by 18-20%
- increase HDL by 1-5%
- decrease TGs by 5-11%
- contraindicated in liver diseases
Omega-3 fatty acids:
- reduce hepatic production of TGs
- modestly reduce LDL and increase HDL
- associated with increased risk of bleeding and decrease in glucose control
Approach to treatment:
Therapy depends on the LDL goal as shown in the figure below
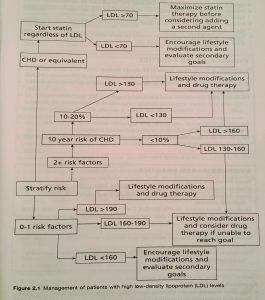
- once LDL goal is achieved then HDL and TGs levels can be considered.
- statins are the first line drugs, treatment shall be started with a low dose (10-20mg) to assess lipid-lowering effect and tolerability, then shall be titrated gradually.
- a second agent may be added if lipid goal is not achieved even with a maximum dose
Complimentary and Alternative Therapies:
- Plant sterols/stenols reduce LDL but not TGs, HDL.
- Soluble fibers has modest lowering effect on Total Cholesterol (TC), LDL.
- Soy protein has modest effect on lowering of TC, LDL, TGs.
- Guggul has also been shown to reduce TC, LDL, TGs.
- Note: all of the above supplements can cause GI upsets
- Red yeast rice, both in capsules and extract form, reduce TC and LDL with no known significant adverse effects
Clinical Pearls:
- LDL shall be treated first before considering secondary goals.
- Patients with CHD can take more benefit from statins
- Patients with acute MI shall early start statins regardless of the LDL levels
- Different statins shall be started before switching to or adding other agents
- Patient profile of creatinine phosphokinase shall only be obtained when muscles pain is experienced
- Pre-medication with aspirin and gradual titration of the dose is advised to improve the effects of Niacin
- If TG>1000 hospitalize the patient and start fibrate urgently
References:
A Practical Approach to Cardiovascular Medicine, First Edition. Edited by Reza Ardehali, Marco Perez, Paul Wang. @2011Blafkwell Publishing Ltd. Published 2011by Blackwell Publishing Ltd.
